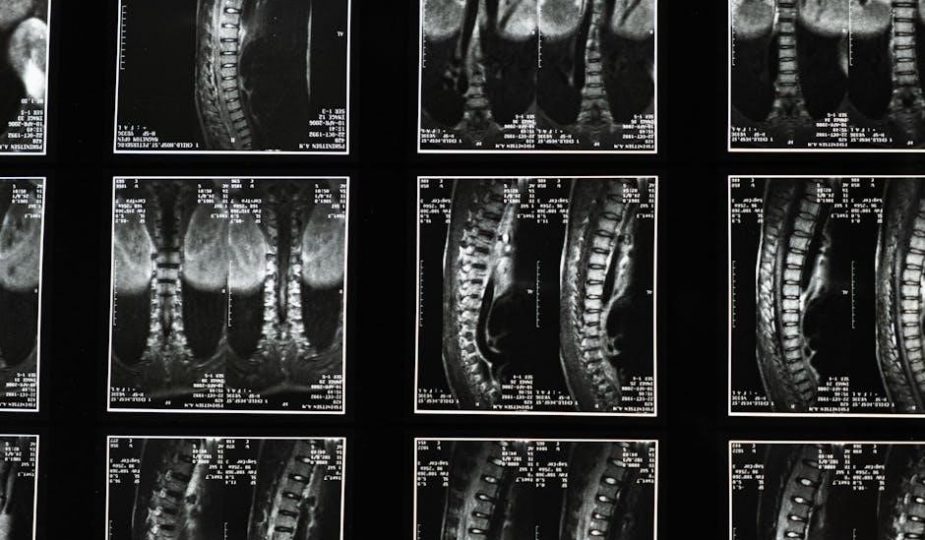
manual spinal decompression
Manual spinal decompression emerges as a promising, non-invasive approach to back pain, offering relief and improved function for many patients seeking alternatives․
This therapy, gaining traction in locations like Helensvale, Australia, focuses on alleviating pressure along the spine, addressing conditions like disc bulges and herniations․
It represents a shift towards conservative care, providing a viable option for those wishing to avoid surgical interventions for chronic back pain and related issues․
What is Manual Spinal Decompression?
Manual Spinal Decompression (MSD) is a specialized, hands-on therapeutic technique utilized to reduce pressure within the spinal column․ Unlike automated traction, MSD relies on the skilled application of precise, rhythmic movements by a trained practitioner․ This gentle, yet effective, method aims to create negative pressure within the intervertebral discs․
This negative pressure is crucial as it encourages the return of vital nutrients and fluids into the discs, promoting healing and reducing inflammation․ Essentially, MSD works by gently “distracting” or separating the vertebrae, relieving compression on nerves and other sensitive structures․ It’s a non-surgical approach focused on restoring proper spinal biomechanics and function․
Practitioners, such as those at Chiro One Helensvale, carefully assess each patient to determine the appropriate techniques and forces needed․ MSD isn’t a one-size-fits-all treatment; it’s tailored to the individual’s specific condition and needs, offering a personalized path to pain relief and improved quality of life․
Historical Context of Spinal Decompression
The roots of spinal decompression trace back to early 20th-century chiropractic and osteopathic practices, where manual traction techniques were employed to address musculoskeletal imbalances․ While not initially termed “decompression,” the core principle of relieving pressure on the spine was present․ Early methods often involved sustained, static stretches․
Over time, advancements in understanding spinal biomechanics led to refinements in these techniques․ The late 20th and early 21st centuries witnessed the development of mechanical decompression devices, aiming to automate and standardize the process․ However, a resurgence of interest in manual techniques emerged, recognizing the nuanced skill and adaptability a practitioner provides․
Today, MSD represents a blend of traditional principles and modern understanding․ It acknowledges the limitations of purely mechanical approaches, emphasizing the importance of a hands-on assessment and individualized treatment plan, as practiced in centers like Chiro One Helensvale, offering a more holistic approach to spinal health․
The Growing Need for Non-Surgical Back Pain Solutions
A significant rise in chronic back pain prevalence fuels the demand for effective, non-surgical interventions like manual spinal decompression (MSD)․ Traditional treatments often fall short, and many patients express reluctance towards invasive procedures, driving exploration of conservative options․
Factors contributing to this trend include an aging population, increasingly sedentary lifestyles, and a greater awareness of the risks associated with surgery․ Patients actively seek alternatives that offer pain relief, improved function, and enhanced quality of life without the downtime and potential complications of surgical interventions․
MSD addresses this need by providing a viable pathway to manage conditions like disc bulges, offering a non-invasive approach, as highlighted by practices such as Chiro One Helensvale․ This growing preference for conservative care positions MSD as a crucial component of modern back pain management․
Understanding Spinal Issues Addressed by Decompression
Manual spinal decompression effectively targets disc problems – bulges, protrusions, and herniations – alongside degenerative disc disease and spinal stenosis, easing related discomfort․
Disc Bulge and Protrusion
Disc bulges and protrusions are common spinal issues frequently addressed with manual spinal decompression therapy․ Unlike a herniation where the disc material breaks through the outer layer, a bulge or protrusion signifies a wider expansion of the disc beyond its normal space․
This expansion can irritate nearby nerves, leading to localized or radiating pain, often felt in the lower back, buttocks, and legs․ At Chiro One Helensvale, practitioners specifically focus on providing effective solutions for individuals experiencing pain stemming from these disc conditions․
Manual decompression works by gently creating negative pressure within the spinal disc, encouraging the bulge or protrusion to retract and relieving pressure on the affected nerves․ This non-invasive approach aims to restore proper spinal alignment and function, reducing pain and improving overall mobility․ The therapy offers a conservative alternative to more invasive interventions․
Herniated Discs
Herniated discs, a more severe form of disc damage than bulges, also respond positively to manual spinal decompression․ A herniation occurs when the soft, gel-like center of the disc breaks through the tough outer layer, potentially compressing spinal nerves and causing significant pain․
This compression can manifest as sciatica – radiating pain down the leg – or localized back pain, impacting daily activities․ Spinal decompression therapy aims to alleviate this pressure by creating a negative intradiscal environment․
This gentle traction encourages the herniated material to retract, reducing nerve irritation and inflammation․ The non-surgical approach offered at clinics like BackFit Health Spine provides a viable option for managing chronic back pain associated with herniated discs․ Manual techniques focus on restoring proper spinal biomechanics and promoting natural healing processes, offering patients a path towards pain relief and improved function․
Degenerative Disc Disease
Degenerative Disc Disease (DDD) isn’t a disease, but rather a gradual breakdown of the spinal discs due to wear and tear․ This can lead to pain, stiffness, and reduced range of motion․ Manual spinal decompression offers a targeted approach to managing DDD symptoms by restoring hydration and space within the affected discs․
By gently creating traction, the therapy aims to reduce pressure on the discs, allowing nutrient exchange and potentially slowing the degenerative process․ This can alleviate pain and improve spinal function, offering a non-surgical alternative to managing chronic discomfort․
Clinics like Chiro One Helensvale emphasize providing effective solutions for DDD sufferers, focusing on individualized treatment plans․ The goal is to enhance quality of life by addressing the underlying spinal mechanics and promoting long-term stability, rather than simply masking the symptoms․
Spinal Stenosis
Spinal Stenosis involves a narrowing of the spinal canal, often causing pressure on the spinal cord and nerves, leading to pain, numbness, and weakness․ Manual spinal decompression presents a potential therapeutic avenue for managing this condition by gently widening the spaces within the spine․
The traction and distraction techniques employed aim to relieve pressure on the compressed nerves, reducing associated symptoms and improving neurological function․ This non-invasive approach can be particularly beneficial for patients seeking alternatives to surgery, offering a chance to regain mobility and reduce discomfort․
Providers in areas like Helensvale, Australia, are increasingly incorporating decompression therapy into their treatment protocols for spinal stenosis․ The focus is on restoring optimal spinal biomechanics and enhancing the patient’s overall well-being through targeted, individualized care․

The Principles of Manual Spinal Decompression
Manual spinal decompression utilizes precise, hands-on techniques to create negative pressure within the spine, promoting disc healing and relieving nerve compression effectively․
How it Differs from Traditional Chiropractic Adjustments
Traditional chiropractic adjustments primarily focus on restoring joint mobility and reducing nerve irritation through high-velocity, low-amplitude (HVLA) thrusts․ While effective for certain musculoskeletal issues, this approach differs significantly from manual spinal decompression․
Decompression, conversely, emphasizes gentle, sustained traction to create space between vertebral segments․ This reduces pressure on intervertebral discs and nerves, facilitating healing and reducing pain․ Unlike the quick, forceful movements of adjustments, decompression is a slower, more controlled process․
Adjustments aim to correct misalignments (subluxations), while decompression targets disc pathology and nerve compression directly․ Decompression doesn’t necessarily correct a misalignment, but rather creates an environment for the body to heal despite potential structural issues․ Both modalities can be beneficial, but they address different mechanisms of pain and dysfunction, making them often complementary rather than interchangeable․
The Role of Traction and Distraction
Traction and distraction are fundamental principles underpinning manual spinal decompression․ Traction involves a gentle, sustained pulling force applied to the spine, aiming to separate vertebral segments․ This creates negative pressure within the intervertebral discs, encouraging fluid and nutrient exchange – crucial for healing damaged tissues․
Distraction, a related concept, specifically refers to the widening of the space between vertebrae․ Manual therapists achieve this through skilled hands-on techniques, carefully positioning and mobilizing the spine․ This differs from simple stretching; it’s a precise application of force designed to reduce compression on nerves and discs․
The combined effect of traction and distraction alleviates pain, improves spinal mobility, and promotes the body’s natural healing processes․ It’s a biomechanical approach focused on restoring optimal spinal function by addressing the root cause of discomfort, rather than merely masking symptoms․
Neuromechanical Effects on the Spine
Manual spinal decompression exerts significant neuromechanical effects on the spine, impacting both the nervous system and the biomechanical structures․ The reduction in pressure on spinal discs and nerves facilitates improved nerve conduction and reduces irritation of sensitive tissues․
This decompression creates a more favorable environment for nerve function, potentially alleviating radiating pain, numbness, and weakness․ Mechanically, the separation of vertebral segments restores proper joint movement and reduces muscle spasm, enhancing spinal flexibility․
Furthermore, the negative pressure generated within the discs encourages fluid exchange, bringing nutrients and removing waste products, promoting disc health and regeneration․ These combined effects contribute to pain reduction, improved function, and a restoration of the spine’s natural biomechanics, offering a holistic approach to spinal health․
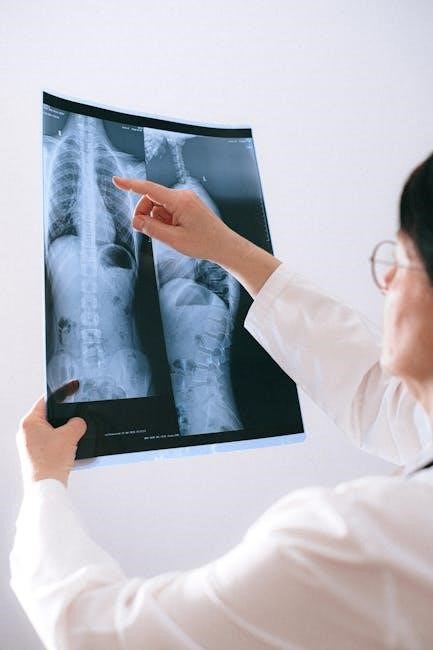
The Manual Spinal Decompression Procedure
Manual spinal decompression begins with a thorough patient assessment, followed by carefully applied techniques to gently stretch and reposition the spine for optimal results․
Patient Assessment and Evaluation
A comprehensive patient assessment is the cornerstone of effective manual spinal decompression therapy․ This initial evaluation goes beyond simply identifying the location of pain; it delves into the patient’s complete medical history, including previous injuries, surgeries, and existing health conditions․
Practitioners will conduct a detailed neurological and orthopedic examination, assessing range of motion, reflexes, muscle strength, and sensory function․ Specific attention is given to postural analysis and palpation to identify areas of spinal dysfunction and soft tissue restrictions․
Imaging studies, such as X-rays or MRIs, may be reviewed to confirm the diagnosis and rule out any contraindications to treatment․ Understanding the root cause of the patient’s pain – whether it stems from a disc bulge, herniation, or degenerative disc disease – is crucial for tailoring a personalized treatment plan․ This meticulous approach ensures the safety and efficacy of the decompression process․
Treatment Positioning and Techniques
Manual spinal decompression utilizes specific positioning and skilled techniques to achieve optimal results․ Patients are typically treated while lying prone or supine on a comfortable, padded table, allowing for relaxed muscle tone and improved access to the spine․
The practitioner employs a gentle, rhythmic oscillation combined with sustained traction forces․ These forces are carefully applied to specific spinal segments, creating a negative pressure within the intervertebral discs․ This decompression aims to reduce pressure on nerves and promote fluid exchange, facilitating healing․
Skilled hand placement and precise movements are essential, differing significantly from traditional chiropractic adjustments․ Therapists often incorporate soft tissue mobilization techniques to address surrounding muscle imbalances and enhance treatment effectiveness․ The goal is to restore proper spinal biomechanics and alleviate pain without causing further irritation․
Typical Session Duration and Frequency
Manual spinal decompression sessions generally range from 30 to 60 minutes in duration, allowing sufficient time for a thorough assessment, targeted treatment, and post-treatment advice․ The initial sessions may focus on gentle mobilization and assessing the patient’s response to the techniques․
A typical treatment plan involves a series of sessions, often ranging from 6 to 12 visits, scheduled 2-3 times per week․ This frequency allows for consistent decompression and cumulative effects on the spinal structures․ The exact number of sessions is individualized based on the severity of the condition, patient response, and overall health status․
Progress is regularly monitored, and the treatment plan is adjusted accordingly․ Maintenance sessions may be recommended following the initial course to sustain improvements and prevent recurrence of symptoms, ensuring long-term spinal health․
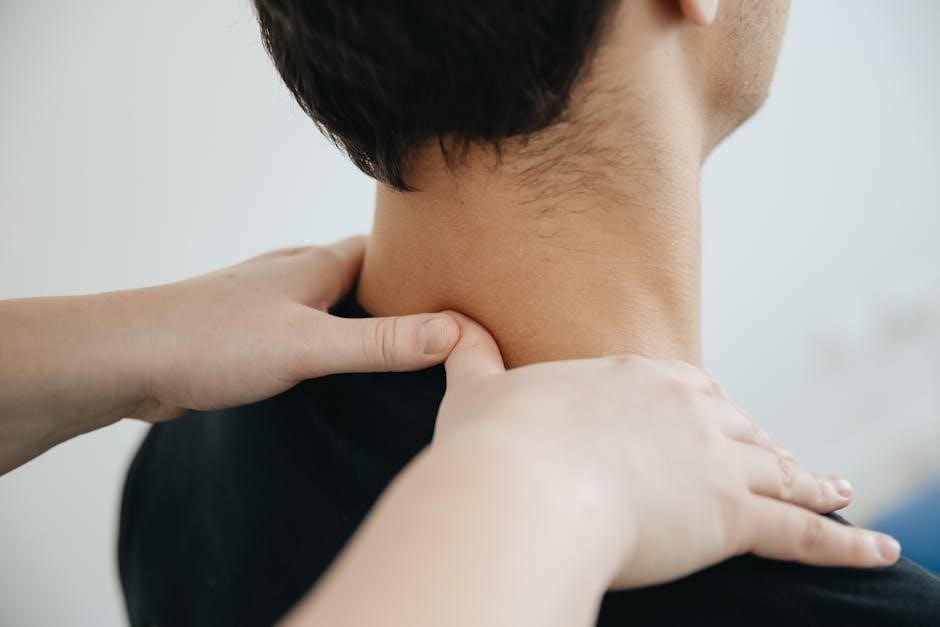
Benefits of Manual Spinal Decompression
Manual spinal decompression demonstrably reduces pain, enhances spinal function and mobility, and ultimately improves patients’ overall quality of life through non-invasive care․
Pain Reduction and Management
Manual spinal decompression excels in its ability to significantly reduce pain associated with various spinal conditions․ By gently relieving pressure on spinal discs and nerves, the therapy addresses the root cause of discomfort, rather than merely masking symptoms․
Patients experiencing lower back pain, often stemming from disc bulges or herniations, frequently report substantial improvements in pain intensity following a series of decompression sessions․ This reduction in pain allows for increased activity levels and a return to daily routines previously hindered by discomfort․
Furthermore, the therapy promotes the body’s natural healing processes, contributing to long-term pain management․ Unlike some pain relief methods, manual decompression aims to create a sustainable solution, empowering individuals to regain control over their spinal health and minimize reliance on medication or more invasive procedures․ The focus is on restoring optimal spinal biomechanics and reducing nerve irritation, leading to lasting pain relief․
Improved Spinal Function and Mobility
Manual spinal decompression doesn’t just address pain; it actively works to restore optimal spinal function and mobility․ By creating space between vertebrae, the therapy alleviates compression on nerves and allows for a greater range of motion․ This is particularly beneficial for individuals experiencing stiffness or limited movement due to degenerative disc disease or spinal stenosis․
As pressure is reduced, muscles surrounding the spine can relax, further enhancing flexibility and reducing muscle spasms․ Improved spinal function translates to better posture, easier movement, and a decreased risk of re-injury․ Patients often find they can perform everyday activities – bending, lifting, twisting – with greater ease and less discomfort․
The therapy’s focus on restoring biomechanical integrity supports the spine’s natural ability to move and function correctly, promoting long-term health and preventing further deterioration․ This holistic approach contributes to a more active and fulfilling lifestyle․
Enhanced Quality of Life
Manual spinal decompression extends its benefits far beyond mere pain reduction, profoundly enhancing a patient’s overall quality of life․ By addressing the root causes of spinal discomfort, individuals often regain the ability to participate in activities they previously avoided due to pain, such as hobbies, exercise, and social engagements․
Reduced pain and improved mobility contribute to better sleep, increased energy levels, and a more positive outlook․ The ability to perform daily tasks without constant discomfort significantly reduces stress and improves mental well-being․ Patients report feeling more independent and capable, leading to greater self-confidence․
Ultimately, successful spinal decompression empowers individuals to reclaim their lives, fostering a renewed sense of freedom and enjoyment․ This holistic improvement in physical and emotional health represents a significant and lasting benefit․

Comparing Manual vs․ Mechanical Spinal Decompression
Manual techniques offer personalized treatment, adapting to individual needs, while mechanical devices provide standardized protocols; both aim to relieve spinal pressure effectively․
Advantages of Manual Techniques
Manual spinal decompression distinguishes itself through a highly individualized approach to patient care․ Unlike mechanical devices that follow pre-programmed settings, a skilled practitioner can dynamically adjust treatment based on real-time patient feedback and nuanced anatomical assessments․
This adaptability allows for a more precise targeting of specific spinal segments and dysfunctional tissues․ The practitioner’s hands-on approach fosters a deeper understanding of the patient’s unique biomechanics, enabling subtle yet impactful adjustments that optimize therapeutic outcomes․
Furthermore, manual decompression often integrates with other therapeutic modalities, such as soft tissue mobilization and targeted exercises, creating a holistic treatment plan․ This comprehensive strategy addresses not only the symptoms but also the underlying causes of spinal dysfunction, promoting long-term stability and improved function․ The tactile feedback provided during manual therapy also allows for a stronger patient-practitioner connection, enhancing trust and compliance․
Limitations of Mechanical Devices
Mechanical spinal decompression, while offering a standardized approach, can present certain limitations compared to manual techniques․ These devices often operate on pre-set protocols, lacking the dynamic adaptability crucial for addressing individual patient variations in anatomy and pain presentation․
The absence of real-time tactile feedback restricts the practitioner’s ability to fine-tune treatment based on the patient’s immediate response․ This can lead to a less precise application of traction forces, potentially diminishing therapeutic effectiveness․
Moreover, mechanical devices typically focus solely on spinal distraction, neglecting the importance of addressing surrounding soft tissues and muscular imbalances․ A holistic approach, integrating manual therapy with exercise and mobilization, is often more effective for long-term pain relief and functional restoration․ Reliance on a machine can also reduce the crucial patient-practitioner connection, potentially impacting treatment adherence and overall outcomes․
Cost-Effectiveness Analysis
Evaluating the cost-effectiveness of manual versus mechanical spinal decompression requires considering both initial expenses and long-term outcomes․ While mechanical devices represent a significant upfront investment for clinics, manual therapy’s cost is primarily linked to the practitioner’s time and expertise․
Manual techniques often require fewer overall sessions to achieve comparable results, potentially reducing the total treatment expenditure for patients․ Furthermore, the holistic nature of manual decompression – addressing soft tissues and movement patterns – may lead to more durable improvements, decreasing the likelihood of recurrent pain and future healthcare costs․
Considering the potential for reduced reliance on pain medication and avoidance of costly surgical interventions, manual spinal decompression presents a compelling value proposition․ A thorough cost-benefit analysis should factor in not only direct treatment costs but also indirect expenses like lost workdays and diminished quality of life․
Contraindications and Precautions
Spinal decompression isn’t suitable for everyone; certain conditions like fractures, infections, or advanced osteoporosis necessitate caution and careful patient screening․
Conditions Where Decompression is Not Recommended
Manual spinal decompression, while beneficial for many, presents contraindications for specific health conditions, demanding careful patient evaluation before commencement․ Active spinal infections are a firm exclusion, as decompression could potentially spread the infection․ Similarly, individuals with spinal fractures or acute fractures require stabilization before any decompression therapy is considered․
Patients with advanced osteoporosis, characterized by significantly reduced bone density, may be at increased risk of vertebral compression fractures during the traction phase․ Furthermore, those with spinal tumors, whether benign or malignant, should not undergo decompression, as it could exacerbate their condition․
Individuals with severe vascular compromise, such as aortic aneurysms, or those with active inflammatory conditions affecting the spine are also generally not suitable candidates․ Finally, pregnancy is a relative contraindication, and decompression should be avoided during this period due to potential risks to the developing fetus․
Potential Risks and Side Effects
Manual spinal decompression is generally considered safe, but, like any therapeutic intervention, it carries potential, albeit typically mild, risks and side effects․ The most commonly reported is temporary soreness in the treated area, similar to that experienced after a strenuous workout․ Some patients may experience localized muscle spasms, which usually resolve within 24-48 hours with gentle stretching and hydration․
Headaches are occasionally reported, potentially due to changes in cerebrospinal fluid dynamics during traction․ Rarely, patients may experience temporary numbness or tingling in the extremities, which typically subsides quickly․ It’s crucial to report any persistent or worsening symptoms to the practitioner immediately․
Serious adverse events are extremely uncommon with properly administered manual decompression․ However, pre-existing conditions must be carefully considered to minimize any potential complications․ A thorough medical history is paramount․
Importance of a Thorough Medical History
A comprehensive medical history is absolutely critical before initiating manual spinal decompression therapy․ This detailed assessment allows the practitioner to identify any contraindications or precautions necessary for safe and effective treatment․ Conditions like severe osteoporosis, spinal fractures, active infections, or certain types of cancer may preclude decompression․
Furthermore, understanding the patient’s complete health profile – including pre-existing neurological conditions, medications, and previous surgeries – helps tailor the treatment plan and minimize potential risks․ Open communication regarding pain levels, symptom patterns, and functional limitations is also essential․
A careful evaluation ensures that manual decompression is an appropriate and beneficial option, maximizing positive outcomes and safeguarding patient well-being․ It’s a cornerstone of responsible and ethical practice․
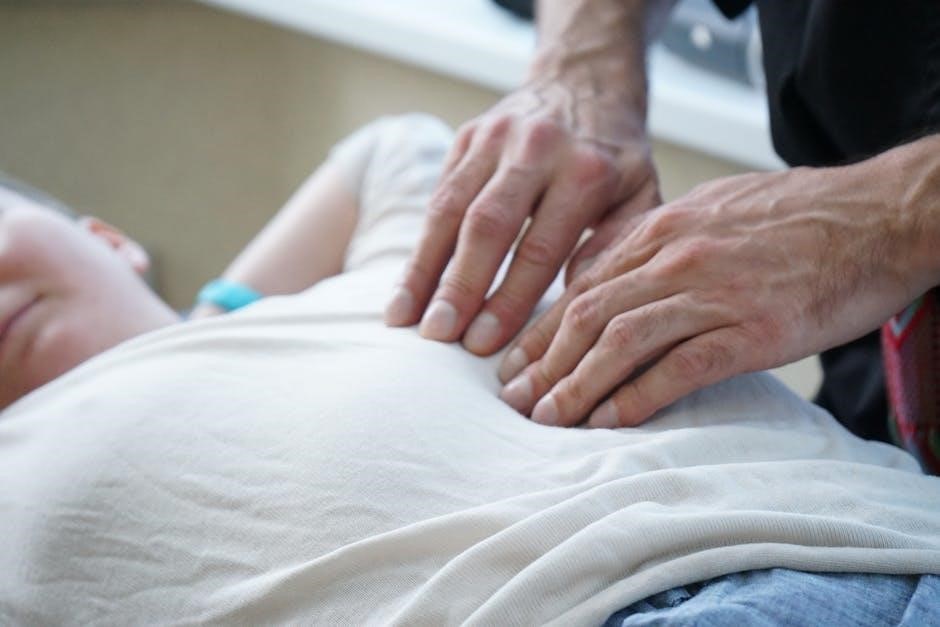
Spinal Decompression in Helensvale, Australia (Specific Location Focus)
Helensvale, Australia, benefits from clinics like Chiro One, specializing in manual spinal decompression for disc issues and chronic back pain relief․
Chiro One Helensvale and its Approach
Chiro One Helensvale distinguishes itself by prioritizing effective, patient-centered solutions for spinal concerns, particularly those stemming from disc bulges and related conditions․ Their approach to manual spinal decompression isn’t simply a treatment; it’s a carefully considered component of a broader wellness strategy․
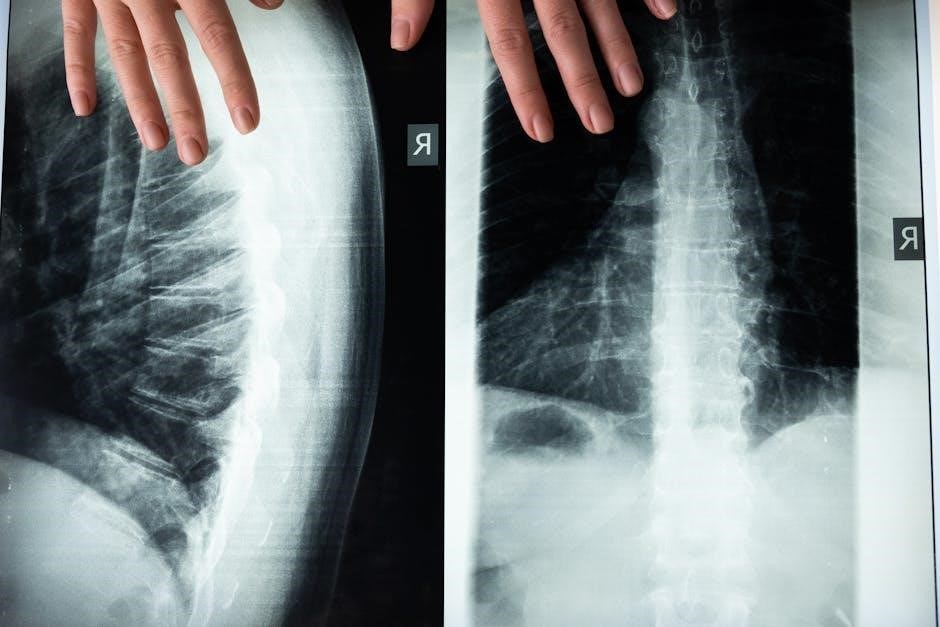
The clinic focuses on providing comprehensive care, beginning with a thorough assessment to accurately diagnose the root cause of a patient’s pain․ This detailed evaluation informs a personalized treatment plan, ensuring the decompression therapy is specifically tailored to individual needs and anatomical considerations․
They emphasize a holistic perspective, recognizing that spinal health impacts overall well-being․ Beyond decompression, Chiro One Helensvale may incorporate other therapies and lifestyle recommendations to support long-term spinal health and prevent recurrence of issues․ Their commitment extends to empowering patients with knowledge and tools for self-management․
Local Availability of Manual Decompression Therapists
Helensvale, Australia, is experiencing growing accessibility to manual spinal decompression therapy, with several clinics now offering this non-surgical treatment option․ While Chiro One Helensvale is a prominent provider, other healthcare facilities, such as BackFit Health Spine, are also integrating spinal decompression into their services․
Finding a qualified therapist requires careful consideration․ Patients should seek practitioners with specific training and experience in manual spinal decompression techniques, ensuring they possess a deep understanding of spinal biomechanics and patient assessment․
Online directories and local healthcare networks can assist in identifying qualified therapists in the Helensvale area․ It’s advisable to verify credentials and read patient reviews before scheduling a consultation․ The increasing availability reflects a rising demand for effective, non-invasive back pain solutions within the community․
Patient Testimonials and Success Stories (Helensvale)
Patient experiences with manual spinal decompression in Helensvale consistently highlight significant reductions in pain and improvements in overall quality of life․ Many individuals, previously struggling with chronic lower back pain due to disc bulges, report increased mobility and a return to daily activities․
Testimonials frequently mention the non-invasive nature of the therapy as a key benefit, offering a welcome alternative to surgery․ Patients at Chiro One Helensvale specifically praise the thorough assessment process and personalized treatment plans․
Success stories often detail a gradual decrease in pain intensity, allowing patients to reduce reliance on pain medication․ Improved function, such as bending, lifting, and walking, are commonly reported outcomes, demonstrating the therapy’s positive impact on physical well-being within the Helensvale community․







